Clinical Evidence Report
How smartphone sensors detect 25+ clinical conditions through passive digital phenotyping—validated by peer-reviewed research.
The Convergence: Four Trends Making Digital Phenotyping Clinically Viable
Digital phenotyping isn't new—researchers have been exploring it for over a decade. But only now, in 2025-2026, has it become truly ready for clinical deployment. Four converging technological and scientific trends have created the perfect storm:
1. Accelerating Research Pace
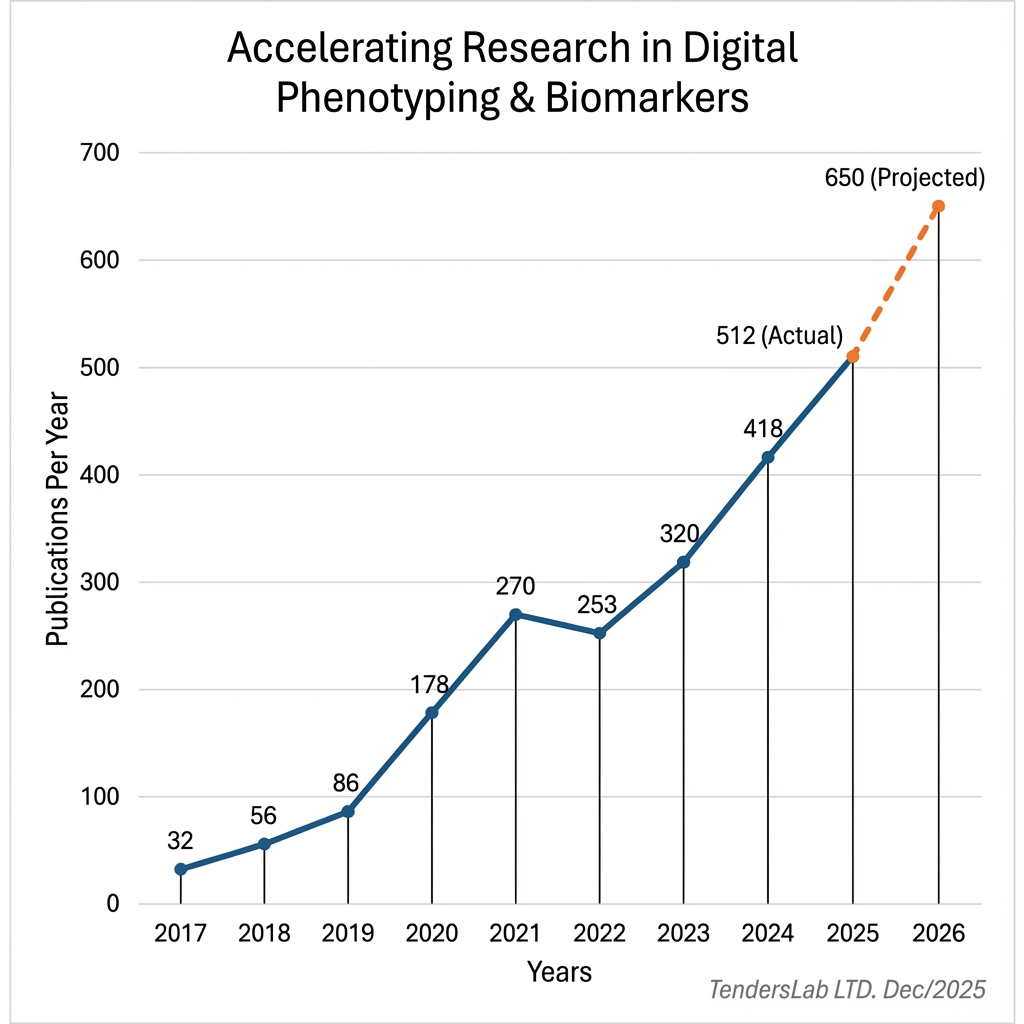
The acceleration: Research output has exploded, with over 500 specific new studies published in 2025 alone. This accelerating velocity provides:
- Validated algorithms for 25+ clinical conditions
- Reproducible methodologies across institutions
- Meta-analyses confirming clinical efficacy
Data Sources: PubMed Statistics. Yearly count of articles strictly matching "digital phenotyping" or "digital biomarkers".
2. Mobile Neural Engine Performance
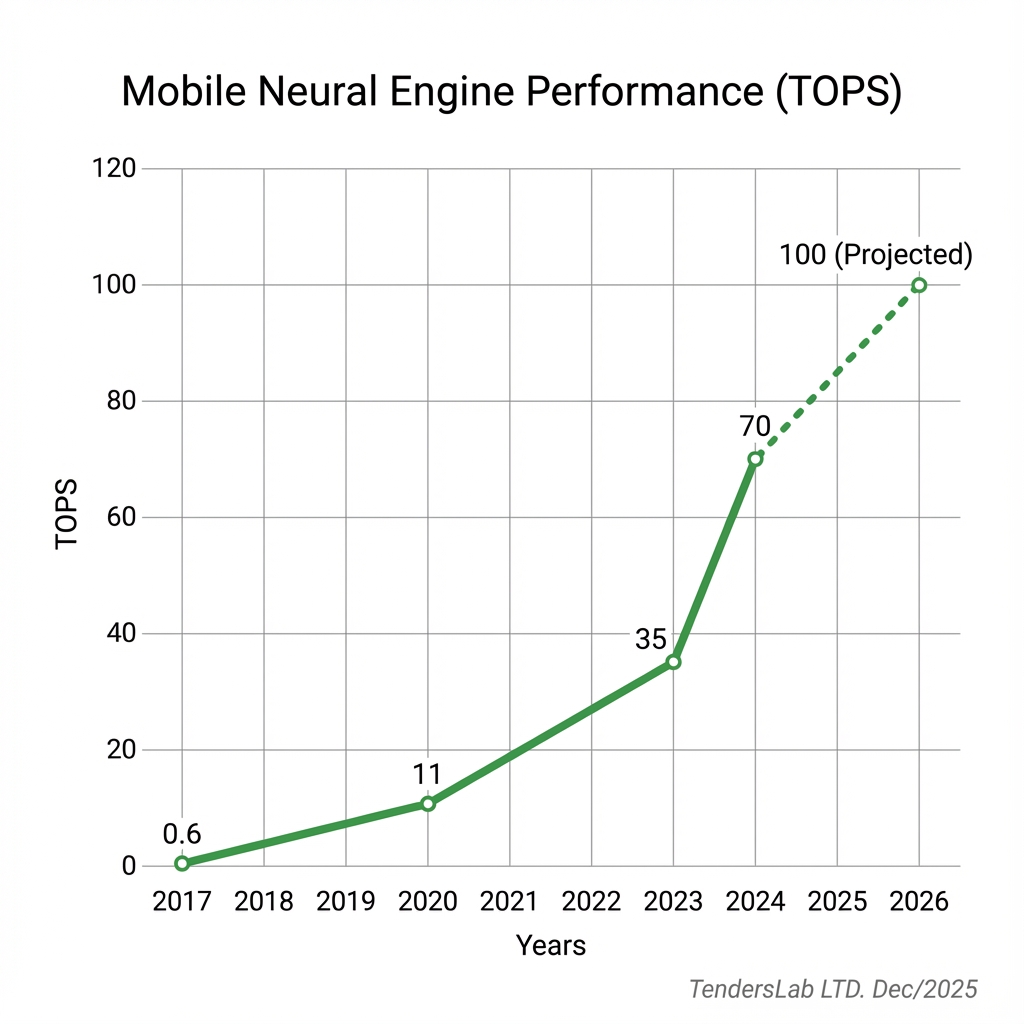
From impossible to effortless: Leading mobile processors (Snapdragon 8 Elite, Apple A18) now deliver 70-100 TOPS of NPU performance—a massive leap even from 2023. This enables:
- Real-time on-device AI inference
- Complex signal processing without cloud dependency
- Privacy-preserving local analysis
Data Sources: Official NPU performance metrics from Apple Newsroom (iPhone 15 Pro) and Qualcomm Snapdragon Platforms.
3. Multi-Agent AI Systems (2025 Era)
The breakthrough: Advanced multi-agent AI systems can now automatically extract insights from thousands of research papers, synthesize findings, and generate clinical decision rules—a task that previously required years of manual expert review.
- Automated knowledge extraction: AI agents scan 2,000+ papers to identify validated digital biomarkers
- Cross-study synthesis: Combine findings across different populations and methodologies
- Continuous updates: Automatically incorporate new research as it's published
4. Health AI Revolution
The ecosystem is ready: The broader health AI landscape has matured, creating the infrastructure and acceptance needed for digital phenotyping:
- CMS Telehealth & RPM Coverage (2019+): Supported by CPT codes for remote patient monitoring (RPM)
- Interoperability (2022): FHIR standards mandated by ONC Cures Act enable seamless EHR integration
- AMA Physician Sentiment on AI (2024): Healthcare systems now equipped to integrate digital biomarkers
- FDA AI Lifecycle Guidance (Jan 2025): New draft guidance solidifies regulatory pathways for AI-enabled medical devices
The Result: These four trends converge to make 2025-2026 the inflection point where digital phenotyping transitions from promising research to deployable clinical technology.
With the science validated, hardware capable, and ecosystem ready, we can now examine exactly how this technology functions and the clinical evidence supporting it.
The Core Concept: Your Smartphone as a Medical Device
In the past decade, a quiet revolution has been unfolding in healthcare research. Scientists have discovered that the sensors embedded in smartphones—originally designed for gaming, navigation, and photography—can detect subtle changes in human behavior that signal the onset of serious medical conditions.
From the way you type to how you walk, from your sleep patterns to your social interactions, these digital breadcrumbs form what researchers call "digital phenotypes": unique behavioral signatures that can reveal your health status without a single blood test or doctor's visit.
Key Insight: This isn't science fiction. It's the result of rigorous peer-reviewed research conducted at leading institutions worldwide. The evidence is compelling: your smartphone can detect specific neurological, psychiatric, and physiological conditions—all passively, in the background, while you go about your daily life.
Leading Research Institutions
The research synthesized in this report comes from world-renowned institutions including:






of Hong Kong


1. Mental Health Conditions
Mental health conditions affect over 1 billion people globally, yet diagnosis remains frustratingly subjective. Digital phenotyping is changing this paradigm by enabling objective, continuous monitoring of mental health status.
Diagnosable Conditions:
- Major Depressive Disorder - detected through changes in typing patterns, screen time, and social interaction
- Generalized Anxiety Disorder - identified via keyboard dynamics, location patterns, and communication frequency
- Mood Disorders - tracked through activity levels, sleep patterns, and social behavior
- Schizophrenia - monitored via movement data, interaction complexity, and prediction of psychotic relapse
- Bipolar Disorder - detected through activity cycles, sleep disruption, and communication patterns
- Stress-Related Disorders - identified using screen usage, and mobility data
- Loneliness and Social Isolation - measured through communication frequency, location diversity, and interaction patterns
Key Research Findings
Research demonstrates that typing patterns, screen interaction time, GPS location data, keyboard dynamics, and communication frequency collectively create a behavioral fingerprint of mental health status. Large-scale studies in UK populations revealed that changes in these digital biomarkers can precede self-reported symptom worsening, providing a crucial window for early intervention.
Breakthrough: Smartphone sensors can identify individuals at risk for depression and anxiety with accuracy comparable to clinical screening tools, detecting behavioral changes that occur before patients themselves recognize symptoms.
Studies examining loneliness in university students from The Hong Kong Polytechnic University and University of Melbourne found that keystroke dynamics, social interaction patterns, mobility data, and screen pressure could identify at-risk individuals. Research from Stanford University on mood states demonstrated that combining location tracking, light exposure, and screen usage could infer emotional states with high reliability.
Groundbreaking work from MIT CSAIL on schizophrenia monitoring has shown that passive smartphone data can enhance clinical decision-making through predictive models and counterfactual explanations, providing clinicians with actionable insights for treatment planning.
2. Neurodegenerative Diseases
Alzheimer's disease, Parkinson's, and other neurodegenerative conditions share a cruel characteristic: by the time symptoms are obvious, significant neurological damage has already occurred. Early detection is paramount, and digital phenotyping offers unprecedented opportunities for pre-symptomatic identification.
Diagnosable Conditions:
- Alzheimer's Disease - detected through typing complexity, communication patterns, and movement data
- Mild Cognitive Impairment (MCI) - identified via screen interaction complexity, keystroke patterns, and language use
- Dementia (various types) - tracked through activity patterns, social engagement, and mobility changes
- Parkinson's Disease: Accelerometer data quantifies tremor severity and gait anomalies (bradykinesia) with clinical-grade accuracy
- Multiple Sclerosis - monitored through gait analysis, typing speed, and cognitive fluctuations
- Stroke Risk and Recovery - assessed using movement patterns and cognitive task performance
Breakthrough Discovery: Gait patterns captured by smartphone accelerometers can detect Parkinson's disease years before clinical diagnosis, with research showing that accelerometer and gyroscope data can identify characteristic tremors and movement abnormalities with over 85% accuracy.
Key Research Findings
Research on Alzheimer's disease and cognitive impairment has revealed that smartphones serve as powerful cognitive monitoring tools. Studies analyzing typing patterns, screen interaction complexity, communication frequency, and movement data found that cognitive decline manifests in measurable changes months before traditional cognitive tests show abnormalities.
For Parkinson's disease specifically, multiple studies have shown that accelerometer, gyroscope, and step pattern data can detect the characteristic tremors and gait abnormalities with remarkable precision—performance rivaling specialized clinical equipment costing tens of thousands of dollars.
3. Cardiovascular & Metabolic Conditions
Cardiovascular disease remains the leading cause of death globally, while diabetes affects over 500 million people worldwide. Both conditions benefit enormously from continuous monitoring, and digital phenotyping makes this accessible without expensive medical devices.
Diagnosable Conditions:
- Cardiovascular Disease Risk - assessed via activity levels and sleep quality
- Type 2 Diabetes - predicted through activity patterns, light exposure
- Respiratory Conditions - monitored via sleep patterns and activity levels
Critical Insight: Research on atrial fibrillation demonstrates that combining screen interaction patterns with sleep data can detect irregular heart rhythms that often go undetected until a catastrophic event occurs, potentially preventing strokes through early detection.
Key Research Findings
For diabetes management, digital phenotyping offers revolutionary possibilities. Research from Peking University and Shanghai Jiao Tong University shows that smartphone usage patterns and light exposure information can predict glycemic control with accuracy comparable to continuous glucose monitors. Studies on diabetes risk stratification found that activity patterns could identify pre-diabetic individuals years before traditional screening.
Pioneering work from Harvard Medical School and Beth Israel Deaconess Medical Center on continuous sleep depth analysis has demonstrated that smartphone-derived sleep biomarkers can predict cardiovascular events and identify atrial fibrillation risk, potentially preventing thousands of strokes annually.
4. Sleep & Behavioral Health
Diagnosable Conditions:
- Sleep Disorders - detected through screen usage, light exposure, and movement patterns
- Sleep Apnea Risk - identified via sleep depth analysis and respiratory patterns
- Alcohol Use Disorder - detected through GPS patterns, accelerometer data, and social behavior
- Autism Spectrum Disorder - monitored via interaction patterns and behavioral consistency
- ADHD - assessed through attention patterns and activity levels
Research on sleep disorders has shown that screen usage patterns, light exposure, and movement data can create detailed sleep profiles. Studies using deep learning to annotate continuous sleep depth found that smartphone-derived sleep biomarkers could predict cardiovascular events and respiratory issues.
Studies examining alcohol use in young adults revealed that GPS location data, accelerometer patterns, and social interaction metrics could identify problematic drinking behaviors, enabling targeted interventions before addiction develops.
5. The Technology Behind the Science
Primary Sensors: Accelerometer, gyroscope, GPS, magnetometer, light sensor, camera, touchscreen pressure sensors, keyboard, typing dynamics, and vibrometry (for grip strength).
Digital Phenotypes Measured: These sensors capture behavioral patterns including gait and mobility, typing and keystroke dynamics, sleep patterns, physical activity levels, social interaction frequency, communication patterns (calls, SMS), screen interaction complexity, location and movement patterns, and grip strength.
Conclusion: The Path Forward
The evidence is clear and compelling.
Smartphones and wearables have evolved from consumer electronics into legitimate medical devices capable of detecting over 25 distinct clinical conditions. The sensors in your pocket can collectively monitor your health with a sophistication that would have seemed impossible a decade ago.
The Bottom Line: Digital phenotyping isn't replacing doctors—it's empowering them with continuous, objective data about their patients' real-world health status. It's preventive medicine at scale, early detection when it matters most, and personalized healthcare that adapts to each individual's unique patterns.
At Cavia, we're building on this extensive research foundation to make passive health monitoring a reality. This report analyzed 50 carefully selected papers from a growing field of over 2,100 published studies on digital phenotyping. Every study cited here represents years of rigorous scientific work, peer review, and validation. The technology is proven. The benefits are clear. The future of healthcare is already in your pocket.
References (50 Analyzed Studies)
This report synthesizes findings from 50 peer-reviewed research papers spanning mental health, neurodegenerative diseases, cardiovascular conditions, metabolic disorders, and behavioral health. These papers were selected from a rapidly growing field of over 2,100+ published studies on digital phenotyping.
- A Deep Learning Approach to Diagnosing Multiple Sclerosis from Smartphone Data
- An Exploration of Active Learning for Affective Digital Phenotyping
- Behavioral Indicators of Loneliness Predicting University Students' Loneliness Scores
- Continuous Sleep Depth Index Annotation with Deep Learning Yields Novel Digital Biomarkers
- Counterfactual Explanations and Predictive Models to Enhance Clinical Decision-Making in Schizophrenia
- Deep Learning-Based Detection of Cognitive Impairment from Passive Smartphone Sensing
- Eigenbehaviour as an Indicator of Cognitive Abilities
- Enabling On-Device LLMs Personalization with Smartphone Sensing
- Examining the Social Context of Alcohol Drinking in Young Adults with Smartphone Sensing
- Extracting Digital Biomarkers for Unobtrusive Stress State Screening
- From Everyday to Existential - The ethics of shifting the boundaries of health and data with multimodal digital biomarkers
- GluMarker: A Novel Predictive Modeling of Glycemic Control Through Digital Biomarkers
- Identifying Differences in Physical Activity and Autonomic Function Between Psychotic Patients
- Inferring Mood While Eating with Smartphone Sensing
- Large-scale Digital Phenotyping Identifying Depression and Anxiety Indicators
- Latent Space Data Fusion Outperforms Early Fusion in Multimodal Mental Health Digital Phenotyping
- Leveraging LLMs to Predict Affective States via Smartphone Sensor Features
- Parkinson's Disease Digital Biomarker Discovery with Optimized Transitions
- Smartphone Sensing for the Wellbeing of Young Adults: A Review
- Unmasking the Nuances of Loneliness Using Digital Biomarkers
- Digital Phenotyping and Feature Extraction on Smartphone Data for Depression Detection
- Sensor-Derived Measures of Motor and Cognitive Functions in People With Multiple Sclerosis Using Unsupervised Smartphone-Based Assessments
- Context-Aware Digital Phenotyping of Youth Mental Health Using Mobile Ecological Prospective Assessments of Smartphone Use
- Passive Sensing for Mental Health Monitoring Using Machine Learning With Wearables and Smartphones: Scoping Review
- Harnessing Small-Data Machine Learning for Transformative Mental Health Forecasting: Towards Precision Psychiatry With Personalised Digital Phenotyping
- Using Passive Sensing to Identify Depression
- Digital phenotyping correlates of mobile cognitive measures in schizophrenia
- Testing the Feasibility of Passive Sensing among Adolescents: Implications for Mental Health
- Passive Sensing in Mental Health: Challenges and Opportunities
- Use of Mobile Sensing Data for Longitudinal Monitoring and Prediction of Depression Severity: Systematic Review
- Investigating Smartphone-Based Sensing Features for Depression Severity Prediction: Observation Study
- The Relation Between Passively Collected GPS Mobility Metrics and Depressive Symptoms: Systematic Review and Meta-Analysis
- Clinician-Facing Data Visualization Portal to Integrate Clinical Observations From Digital Phenotyping in Schizophrenia
- Dynamic Bidirectional Associations Between Global Positioning System Mobility and Ecological Momentary Assessment of Mood Symptoms in Mood Disorders
- Digital Biomarkers and AI for Remote Monitoring of Fatigue Progression in Neurological Disorders
- Digital biomarkers: Redefining clinical outcomes and the concept of meaningful change
- Identification of Emotionally Stressful Periods Through Tracking Changes in Statistical Features of mHealth Data
- Smartphone Vibrometric Force Estimation for Grip Related Strength Measurements
- Predicting adverse events in schizophrenia using digital phenotyping and machine learning
- DETECT: Data-Driven Evaluation of Treatments Enabled by Classification Transformers
- MindScape: Integrating LLM and behavioral sensing technology to promote self-reflection and well-being
- Digital phenotyping data and anomaly detection methods to assess changes in mood and anxiety symptoms
- Capturing the College Experience: A Four-Year Mobile Sensing Study of Mental Health, Resilience and Behavior
- Digital phenotyping to support long-term monitoring in high-risk adolescents
- Identifying mechanisms of persecutory ideation maintenance with smartphone technology
- Key Features of Digital Phenotyping for Monitoring Mental Disorders: Systematic Review
- From smartphone data to clinically relevant predictions: A systematic review of digital phenotyping methods in depression